CIED-related tricuspid regurgitation (TR) — particularly pacemaker-induced TR — is an under-recognised but clinically important cause of right heart failure (RHF). While heart failure is most commonly attributed to left ventricular dysfunction, a distinct group of patients presents with primary right-sided pathology involving the right ventricle, right atrium, or tricuspid valve in the absence of left heart disease. Causes include right ventricular ischaemia, arrhythmia, cardiomyopathy, pulmonary hypertension, congenital abnormalities, pulmonary embolism, and tricuspid valve dysfunction. Within this last group, TR caused by cardiac implantable electronic devices (CIEDs) has emerged as an increasingly recognised and clinically significant entity.
- Right vs left heart failure
- TR as a cause of right heart failure
- Mechanisms of CIED-related TR
- Case presentation
- Echocardiogram
- Differentiating CIED-related TR from atrial functional TR
- When to suspect CIED-related TR
- Cardiac CT for lead localisation
- Surgical management and outcome
- Key takeaways
- References
Clinical cautionManaging patients with right heart failure is often challenging — most are elderly with multiple comorbidities, and the risks associated with invasive intervention are substantial. Establishing the precise underlying mechanism and carefully weighing the risk-benefit balance are essential before pursuing any invasive treatment.
Right vs left heart failure: clinical manifestations
Distinct symptoms and signs arise depending on whether the left or right side of the heart is primarily involved. Left heart failure (LHF) is by far the more common presentation and is characterised by fatigue and dyspnoea — initially exertional, and at rest as the disease progresses. Two hallmark features of LHF are orthopnoea and paroxysmal nocturnal dyspnoea (PND). Orthopnoea refers to breathlessness in the recumbent position that is relieved by sitting or standing. PND is characterised by episodes of breathlessness that wake the patient typically 2–4 hours after sleep onset, relieved by sitting up. As LHF progresses, left ventricular and left atrial filling pressures rise and are transmitted back to the pulmonary circulation — producing pulmonary congestion and, in severe cases, pulmonary oedema. Sustained pressure overload of the pulmonary circulation ultimately leads to right ventricular dilatation and failure; LHF is therefore the most common cause of right heart failure (RHF).Differentiating signs and symptoms: right vs left heart failure
In a minority of patients, the primary pathology is confined to the right side of the heart, producing isolated RHF. Typical symptoms include fatigue, abdominal fullness, early satiety, and exertional dyspnoea — reflecting reduced RV stroke volume and impaired pulmonary perfusion. Physical findings that help distinguish RHF from LHF include:- Lung auscultation: crackles from pulmonary congestion are typical of LHF; the chest is usually clear in isolated RHF.
- Hepatomegaly: hepatic congestion from elevated central venous pressure produces a palpable, often tender liver in RHF; hepatomegaly is uncommon in isolated LHF.
- Ascites: fluid accumulation in the peritoneal cavity is considerably more common in RHF.
- Abdominojugular reflux: sustained elevation of the JVP (> 3 cm for > 15 seconds) during firm mid-abdominal compression reflects impaired right heart compliance and is a useful bedside sign of RHF.
Key clinical pointThe hallmark physical findings of RHF are an elevated jugular venous pressure (JVP) and peripheral pitting oedema, particularly in the lower limbs. Early in the course of isolated RHF, the relative absence of PND, orthopnoea, and pulmonary oedema is a key discriminator from the more common LHF.
Tricuspid regurgitation as a cause of right heart failure
Right heart failure is a clinical syndrome arising from impaired function of the right side of the heart, reducing the effective stroke volume delivered to the pulmonary circulation. In tricuspid regurgitation (TR), a variable proportion of right ventricular stroke volume is ejected retrograde into the right atrium during systole rather than forward into the pulmonary artery. Right ventricular systolic function on echocardiography may therefore appear preserved even when effective stroke volume is markedly reduced. As TR severity progresses, the regurgitant fraction rises and the effective forward flow falls further, driving the symptoms of right heart failure.
Aetiological classification of tricuspid regurgitation
Contemporary classification divides TR into four aetiological groups, each with distinct pathophysiology and implications for management.
Primary (organic) TR
Intrinsic structural abnormality of the tricuspid valve apparatus — leaflets, chordae, or papillary muscles. Management is typically directed at the valve itself.
Ventricular functional TR
Structurally normal valve fails to coapt due to RV dilation, dysfunction, or tethering — usually driven by left-sided disease or pulmonary hypertension.
Atrial functional TR
Annular dilation from long-standing atrial fibrillation with preserved biventricular function. Increasingly recognised in elderly populations.
CIED-related TR
Mechanical lead interference and/or pacing-induced RV dysfunction from a pacemaker or defibrillator lead. The focus of this review.
Each group is considered in more detail below.
Primary (organic) TR
Primary TR reflects an intrinsic structural abnormality of the tricuspid valve apparatus itself — the leaflets, chordae, or papillary muscles. Causes include myxomatous degeneration with leaflet prolapse, rheumatic disease, infective endocarditis, carcinoid heart disease, Ebstein anomaly, blunt chest trauma, and iatrogenic injury from endomyocardial biopsy or lead extraction. Primary TR accounts for a minority of clinically significant TR but is important to identify because management is often directed at the valve itself, and earlier surgical intervention is frequently warranted than in secondary forms.
Secondary ventricular (functional) TR
Historically the most common cause of significant TR, ventricular functional TR occurs when a structurally normal valve fails to coapt due to right ventricular dilation, dysfunction, or leaflet tethering. The driver is almost always elevated right-sided pressures — most often from left-sided heart disease (valve disease or heart failure) or pulmonary hypertension of any cause. Management is directed primarily at the underlying left-sided or pulmonary pathology; the TR itself typically improves when RV loading conditions are reduced, although severe or long-standing cases may require intervention.
Secondary atrial (functional) TR
Increasingly recognised as a distinct entity, atrial functional TR arises from right atrial and tricuspid annular dilation in patients with long-standing atrial fibrillation and preserved biventricular function. Unlike ventricular functional TR, the RV is not dilated or dysfunctional — the mechanism is isolated annular enlargement disrupting leaflet coaptation. It is particularly common in elderly patients and has emerged as a significant contributor to the rising burden of TR in ageing populations. Restoration of sinus rhythm, when feasible, can meaningfully reduce TR severity.
CIED-related TR
Tricuspid regurgitation related to cardiac implantable electronic device (CIED) leads is the focus of this review. It arises from two overlapping mechanisms: direct mechanical interference from the lead (impingement, adherence, entanglement, or perforation) and secondary RV dysfunction from chronic right ventricular pacing. The relative contribution of each varies between patients, and distinguishing CIED-induced from CIED-incidental TR is central to management — decisions regarding lead extraction, leadless pacing, cardiac resynchronisation, conduction system pacing, or transcatheter valve intervention all depend on this assessment.
Clinical pearl
Lead-related TR should be suspected when severe TR is present on imaging, but RV size and function appear disproportionately preserved — a pattern that argues against purely functional TR and points to a mechanical lead-leaflet interaction. A high index of suspicion is required, particularly in patients presenting with right heart failure symptoms and a long-standing CIED.
Mechanisms of CIED-related TR
CIED-related tricuspid regurgitation (TR) has been described across multiple observational studies and case series. The proposed mechanisms can be broadly categorised into implantation-related, pacing-related, and lead-mediated factors.- Implantation-related: The risk of tricuspid valve injury at implantation varies with operator technique and final lead position. Crossing the valve through a commissure — rather than directly across a leaflet — and avoiding the septal leaflet where possible are associated with lower rates of subsequent TR. The “prolapsing” technique is generally considered less traumatic than direct leaflet crossing.
- Pacing-related: Chronic right ventricular apical pacing can worsen TR through pacing-induced dyssynchrony, progressive RV remodelling, and secondary tricuspid annular dilation. The magnitude of this effect varies between studies and is typically less pronounced than the mechanical lead-related mechanisms.
- Lead-mediated: Pacemaker or defibrillator leads can interfere with tricuspid valve function through four described mechanisms — impingement, adherence, entanglement, and perforation — as illustrated in Table 1.
| Impingement | The lead mechanically interferes with leaflet mobility and coaptation without direct tethering — the most frequently described mechanism. |
| Adherence | The lead becomes tethered directly to a leaflet, typically through fibrosis and scarring developing over time. |
| Entanglement | The lead becomes caught within the subvalvular apparatus (chordae tendineae), tethering chordal structures rather than the leaflet itself. |
| Perforation | The lead punctures a leaflet during implantation, most commonly affecting the septal leaflet. |
Differentiating impingement from adherence on 2D echocardiography is often challenging; 3D transoesophageal echocardiography with multi-planar reconstruction is the reference standard.
The terminology used to describe lead-related tricuspid valve interactions can overlap, and the mechanisms exist along a continuum rather than as discrete categories. A lead may initially impinge on a leaflet — resting against it without attachment. With time, chronic contact and progressive fibrosis can cause the lead to become adherent, increasingly restricting leaflet motion. By contrast, entanglement within the subvalvular apparatus and perforation of a leaflet are typically distinct events that occur abruptly rather than gradually.
Case presentation

83-year-old man, dual-chamber pacemaker
Progressive exertional dyspnoea and fatigue over three years, with pacemaker-induced severe tricuspid regurgitation on a background of long-standing atrial fibrillation.
History of presenting complaint
An 83-year-old man was referred in 2019 for progressively worsening dyspnoea on exertion and fatigue over the preceding three years. He had no dyspnoea at rest, but his exercise tolerance had declined significantly (NYHA class III), particularly over the previous 12 months. He denied paroxysmal nocturnal dyspnoea or orthopnoea and had no hospital presentations with acute pulmonary oedema — a pattern more consistent with predominant right heart failure. He lived with his partner and remained independent in activities of daily living.
Background
A former professional race-walker, he could comfortably cover 15 km five years earlier but was now struggling to carry groceries from the shops to his car. His only medication was warfarin for long-standing atrial fibrillation, diagnosed in 2000. A permanent pacemaker had been implanted in 2005 for complete heart block. In 2012 he underwent a generator change with insertion of a new ventricular lead; the indication for the new lead was not clear from the available records. An echocardiogram in 2011 showed low-normal left ventricular function, trivial-to-mild tricuspid regurgitation, and a mildly dilated left atrium.
In 2013 — one year after the generator change and new lead — he reported to his cardiologist that "his general health had gone downhill," although he could not elaborate. A repeat echocardiogram at that time showed mild tricuspid regurgitation, mild-to-moderate pulmonary hypertension, and moderately dilated atria. An extended overseas trip then took him out of follow-up for almost five years. His symptoms worsened gradually and were dismissed as "age-related" by family and primary care providers. He had no diabetes, hypertension, or other significant comorbidities, had never smoked, and his renal function was normal.
Physical findings
On presentation in 2019, his blood pressure was 130/70 mmHg and pulse 70 bpm. His chest was mostly clear to auscultation and only mild pitting oedema was present at the ankles. The dominant finding — visible from across the room — was a markedly distended and pulsatile jugular venous pulse, as shown in Video 1.
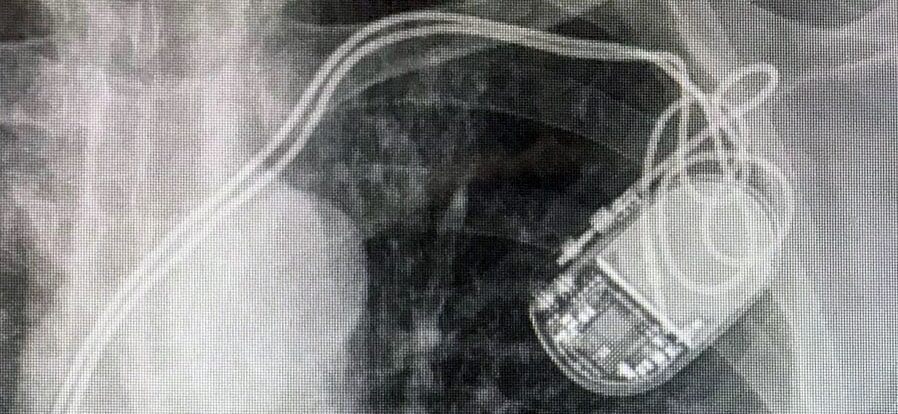
ECG and chest X-ray
The rhythm was paced with underlying atrial fibrillation, with the atrial lead capped. On the PA chest X-ray the right ventricular lead tip lay at the inferior border of the right ventricle; on the lateral view it projected posteriorly — overall consistent with an infero-posterior lead position.
Echocardiogram
The echocardiogram showed grossly dilated atria. LVEF was approximately 50%, with septal dyssynchrony consistent with the paced rhythm. Mild mitral regurgitation was present. The RV was moderately to severely dilated, but RV systolic function was relatively preserved — a pattern that pointed away from purely ventricular functional TR and toward a mechanical lead-mediated mechanism. The TR jet was severe and eccentric, originating from the postero-septal commissure of the tricuspid valve, where the RV pacemaker lead was clearly visible. The lead appeared adherent to the posterior wall of the right ventricle with minimal independent motion, consistent with chronic fibrotic adherence rather than simple impingement.Baseline cardiac function


Tricuspid valve and TR mechanism


Lead–leaflet interaction — the key finding
Differentiating CIED-related TR from atrial functional TR
In this patient, two mechanisms could plausibly explain the severe TR. The first is atrial functional TR — anticipated in a patient with long-standing atrial fibrillation, grossly dilated atria, and preserved biventricular function. The second is CIED-related TR from mechanical lead interaction with the tricuspid valve. In practice, these mechanisms are not mutually exclusive — they often coexist, and distinguishing the dominant contributor is the key to appropriate management. Pure atrial functional TR may respond to rhythm control, diuresis, and afterload reduction; a structural lead–leaflet problem will not.
Clues that favour CIED-related TR as the dominant mechanism
Several features in this case — considered together — point toward a lead-mediated mechanism as the primary driver of the severe TR:
Timeline in relation to the device
The patient’s 2011 echocardiogram — performed when the original 2005 pacemaker leads were still in situ — showed only trivial-to-mild TR. By 2013, one year after generator change and insertion of a new ventricular lead, TR had progressed to mild with new pulmonary hypertension and atrial dilation. Symptom onset correlated temporally with the new lead rather than with the duration of atrial fibrillation, which he had tolerated asymptomatically since 2000. This temporal pattern argues strongly for a lead-related trigger.
Echocardiographic features of the TR jet
Several jet characteristics on imaging favour a lead-mediated rather than purely functional mechanism:
- The TR jet is severe and eccentric, not the central, regurgitant orifice pattern typical of pure annular dilation.
- The jet originates above the coaptation line — a finding specifically associated with lead-mediated mechanisms (leaflet tethering or perforation). Functional annular TR jets arise from failed central coaptation, not from above it.
- The jet hugs the lead, arising immediately adjacent to the RV pacemaker lead at the postero-septal commissure.
Lead characteristics
The RV lead is off-centred, fixed to the postero-septal aspect of the valve, and shows minimal independent motion — moving in concert with the right ventricle rather than freely within the cavity. A healthy uninvolved lead shows independent intracavitary motion distinct from myocardial contraction; this lead does not. This pattern is consistent with one of the four mechanisms of CIED-related TR — most commonly chronic adherence or perforation — developing over the seven-year interval since lead insertion in 2012. 2D transthoracic imaging cannot reliably distinguish adherence from perforation; surgical inspection or 3D transoesophageal echocardiography with multi-planar reconstruction is usually required for definitive mechanistic diagnosis.
Preserved RV systolic function
Despite severe TR and marked RV dilation, RV systolic function is relatively preserved. In long-standing atrial functional TR of this severity, progressive RV dysfunction would typically be expected. A preserved RV in the face of severe TR is a useful pointer toward a primary structural valve problem rather than a chronic functional process — and, importantly, it identifies the patient as a stronger candidate for surgical intervention.
Response to medical therapy
The patient’s RHF symptoms were refractory to diuretic therapy. While diuretic resistance is not specific to CIED-related TR — it is a feature of severe TR of any aetiology — the combination of refractory symptoms with the imaging findings above makes a lead-mediated mechanism the most parsimonious explanation.
Clinical bottom lineTaken together — the temporal correlation with lead insertion, the eccentric lead-hugging jet originating above coaptation, the off-centred minimally mobile lead, the preserved RV function despite severe TR, and the diuretic-refractory symptoms — the dominant mechanism is structural lead–leaflet interaction (chronic adherence or perforation) at the postero-septal commissure. A coexisting atrial functional component from annular dilation is likely given the long-standing AF, but is unlikely to be the primary driver of his severe regurgitation. Definitive distinction between adherence and perforation requires 3D TOE or surgical inspection.
When to suspect CIED-related TR — clinical and imaging clues
The features below are most useful when considered together rather than individually. No single finding is pathognomonic, but the combination of several substantially raises the probability of lead-mediated TR over a purely functional mechanism.
| Clinical or imaging clue | Why it matters |
|---|---|
| Symptom onset after pacemaker implantation or lead change | Temporal correlation with the device suggests a lead-related trigger rather than progression of a pre-existing functional process. |
| Severe TR with relatively preserved RV systolic function | Argues against established ventricular functional TR, in which RV dysfunction would typically be expected at this severity. |
| Eccentric, lead-hugging TR jet on colour Doppler | Suggests mechanical interaction at the lead–leaflet interface; pure annular dilation produces a more central jet. |
| Jet origin above the coaptation line | Specific for lead-mediated mechanisms (leaflet tethering or perforation); functional TR jets arise from failed central coaptation, not from above it. |
| Off-centred lead with minimal independent motion | Lead moving in concert with the right ventricle rather than freely within the cavity is consistent with chronic adherence or perforation. |
| Diuretic-refractory right heart failure | Not specific to CIED-related TR, but in combination with the above raises the probability of a structural rather than purely volume-responsive process. |
| Inability to define the mechanism on 2D TTE | 3D transoesophageal echocardiography with multi-planar reconstruction or surgical inspection is often required to distinguish adherence from perforation. |
Cardiac CT for lead localisation
Although not part of routine CIED-related TR workup, cardiac CT offers cross-sectional confirmation of lead trajectory that plain radiography and echocardiography cannot fully provide. With the expanding use of transcatheter tricuspid valve interventions, CT assessment of lead position relative to the tricuspid annulus and coronary sinus is becoming standard pre-procedural planning — particularly when lead extraction or lead jailing is being considered.
In this patient, cardiac CT confirmed the infero-posterior lead position suggested by the chest X-ray. Rather than crossing the tricuspid annulus centrally — ideally through a commissure — the RV lead was displaced toward the postero-inferior aspect of the valve, directly over the postero-septal commissure where the TR jet originated. This anatomical correlation further supports the lead as the primary driver of the regurgitation.
Surgical management and outcome
Based on the integrated clinical, electrocardiographic, and imaging findings, surgical tricuspid valve replacement was offered. The decision rested heavily on one factor: preserved right ventricular systolic function despite marked chamber dilation. Severe TR with established RV dysfunction carries substantially higher perioperative mortality, and proceeding before RV function declines is a core principle of contemporary tricuspid surgical decision-making.
Operative findings
The patient underwent median sternotomy and tricuspid valve replacement. Direct surgical inspection revealed two mechanisms contributing to the severe TR — confirming the imaging-based suspicion of lead-mediated TR but also identifying a coexisting functional component:
- The RV pacemaker lead had perforated the most inferior portion of the septal leaflet, immediately adjacent to the postero-septal commissure. The lead was deeply embedded within the leaflet and firmly fixed in place — consistent with chronic perforation and surrounding fibrotic encasement.
- The atrial portion of the lead was fibrosed at the cavoatrial junction, precluding straightforward transvenous extraction.
- The tricuspid annulus was markedly dilated to approximately 45 mm (normal < 40 mm), reflecting long-standing atrial fibrillation and right atrial enlargement.
- The remaining tricuspid leaflets were structurally normal.
Pre-operative imaging suggested lead-mediated TR but could not distinguish between adherence and perforation, and underestimated the contribution of the dilated annulus. Surgery confirmed a dual mechanism — chronic lead perforation as the dominant cause, with coexisting atrial functional TR from annular dilation. Multi-mechanism TR is increasingly recognised in patients with long-standing AF and CIED leads, and recognising this pattern matters: pure functional TR may resolve with rhythm control and afterload reduction, but a perforated leaflet will not.
Procedure
A 33 mm bioprosthetic valve was implanted with all native leaflet tissue preserved. Bioprosthetic rather than mechanical valves are standard for tricuspid surgery because of the unacceptably high thrombosis risk with mechanical valves in the low-pressure right heart and to avoid lifelong anticoagulation.
The pacemaker leads were not extracted during the procedure. Transvenous extraction of leads chronically embedded in valve tissue and fibrosed at the cavoatrial junction carries substantial risk — vascular tear, valve disruption, and cardiac perforation — and in an 82-year-old patient who remained pacing-dependent, lead preservation was preferred.
Weaning from cardiopulmonary bypass required moderate inotropic and vasopressor support, reflecting the expected haemodynamic shift after correction of severe TR — loss of the regurgitant "pop-off" produces a sudden rise in RV afterload that often necessitates pharmacological support during the immediate post-bypass period. Haemodynamics stabilised within 30 minutes and the patient was transferred to ICU in a stable condition.
Post-operative course and long-term outcome
The post-operative course was uneventful. Three months after surgery, during cardiac rehabilitation, he completed 9 minutes 34 seconds on the Bruce protocol, reaching a peak workload of 11.0 METs at 83% of age-predicted maximum heart rate — a strong functional result for an 82-year-old. Three years post-operatively, he continues to walk 5–10 km daily without cardiac limitation.
Key takeaways
- In an elderly patient with progressive right-sided heart failure symptoms — fatigue, exertional dyspnoea, abdominal fullness — without orthopnoea or pulmonary oedema, severe TR should be actively sought rather than dismissed as deconditioning or ageing.
- CIED-related TR rarely occurs in isolation. Patients with long-standing AF and a transvenous lead frequently have a multi-mechanism picture combining lead–leaflet interaction with atrial functional TR from annular dilation. Identifying the dominant mechanism guides management.
- The four mechanisms of CIED-related TR (impingement, adherence, entanglement, perforation) cannot be reliably distinguished on 2D transthoracic echocardiography. 3D transoesophageal echocardiography with multi-planar reconstruction or direct surgical inspection is required for definitive mechanistic diagnosis.
- Several echocardiographic features increase the probability of lead-mediated TR: an eccentric jet originating above the coaptation line, a “lead-hugging” jet, an off-centred minimally mobile lead, and preserved RV systolic function out of proportion to TR severity.
- Surgical timing matters. Severe TR with preserved RV function defines the optimal window for intervention; once RV dysfunction is established, perioperative mortality rises substantially. Earlier referral — rather than watchful waiting — improves outcomes.
- Transcatheter tricuspid interventions are evolving rapidly, but feasibility in patients with trans-tricuspid leads depends on lead position, device platform, and operator expertise. Surgical replacement with lead preservation remains the more established option for chronically embedded leads with valve perforation.
References
CIED-related TR — mechanisms, classification, and clinical impact
- Andreas M, et al. Tricuspid valve disease and cardiac implantable electronic devices. Eur Heart J. 2024;45(5):346–365.
- Addetia K, et al. Cardiac implantable electronic device lead-induced tricuspid regurgitation. JACC Cardiovasc Imaging. 2019;12(4):622–636.
- Lin G, et al. Severe symptomatic tricuspid valve regurgitation due to permanent pacemaker or implantable cardioverter-defibrillator leads. J Am Coll Cardiol. 2005;45(10):1672–1675.
- Murphy SP, et al. Cardiac implantable electronic device-induced tricuspid regurgitation: implications and management. Echocardiography. 2024;41(4):e15806.
- Hahn RT, et al. Tricuspid regurgitation: recent advances in understanding pathophysiology, severity grading and outcome. Eur Heart J Cardiovasc Imaging. 2022;23(7):913–929.
Imaging assessment of TR and tricuspid valve anatomy
- Hahn RT, et al. Recommended standards for the performance of transesophageal echocardiographic screening for structural heart intervention. J Am Soc Echocardiogr. 2022;35(1):1–76.
- Mediratta A, et al. 3D echocardiographic location of implantable device leads and mechanism of associated tricuspid regurgitation. JACC Cardiovasc Imaging. 2014;7(4):337–347.
- Zoghbi WA, et al. Recommendations for noninvasive evaluation of native valvular regurgitation. J Am Soc Echocardiogr. 2017;30(4):303–371.
Guidelines on tricuspid valve disease management
- Praz F, et al. 2025 ESC/EACTS guidelines for the management of valvular heart disease. Eur Heart J. 2025.
- Otto CM, et al. 2020 ACC/AHA guideline for the management of patients with valvular heart disease. Circulation. 2021;143(5):e72–e227.
Surgical and transcatheter management
- Sorajja P, et al. Transcatheter repair for patients with tricuspid regurgitation (TRILUMINATE Pivotal). N Engl J Med. 2023;388(20):1833–1842.
- Kar S, et al. Two-year outcomes of transcatheter edge-to-edge repair for severe tricuspid regurgitation: the TRILUMINATE Pivotal randomized controlled trial. Circulation. 2025;151(13):968–981.
- Hahn RT, et al. Transcatheter valve replacement in severe tricuspid regurgitation (TRISCEND II). N Engl J Med. 2025;392(2):115–126.
- Anderson JH, et al. Management and outcomes of transvenous pacing leads in patients undergoing transcatheter tricuspid valve replacement. JACC Cardiovasc Interv. 2020;13(17):2012–2020.
- Kim YJ, et al. Determinants of surgical outcome in patients with isolated tricuspid regurgitation. Circulation. 2009;120(17):1672–1678.
Lead management and the “two-device problem”
- Bashir J, et al. Lead management in patients undergoing percutaneous tricuspid valve replacement or repair: a “heart team” approach. EP Europace. 2023;25(11):euad300.
- The two-device problem: a comprehensive framework for managing transvalvular CIED leads in the era of transcatheter tricuspid intervention. J Clin Med. 2025;14(15):5236.
- Polewczyk A, et al. Long-term follow-up of mortality and heart failure hospitalisation in patients with intracardiac device-related tricuspid regurgitation. Heart Lung Circ. 2021;30(5):692–697.