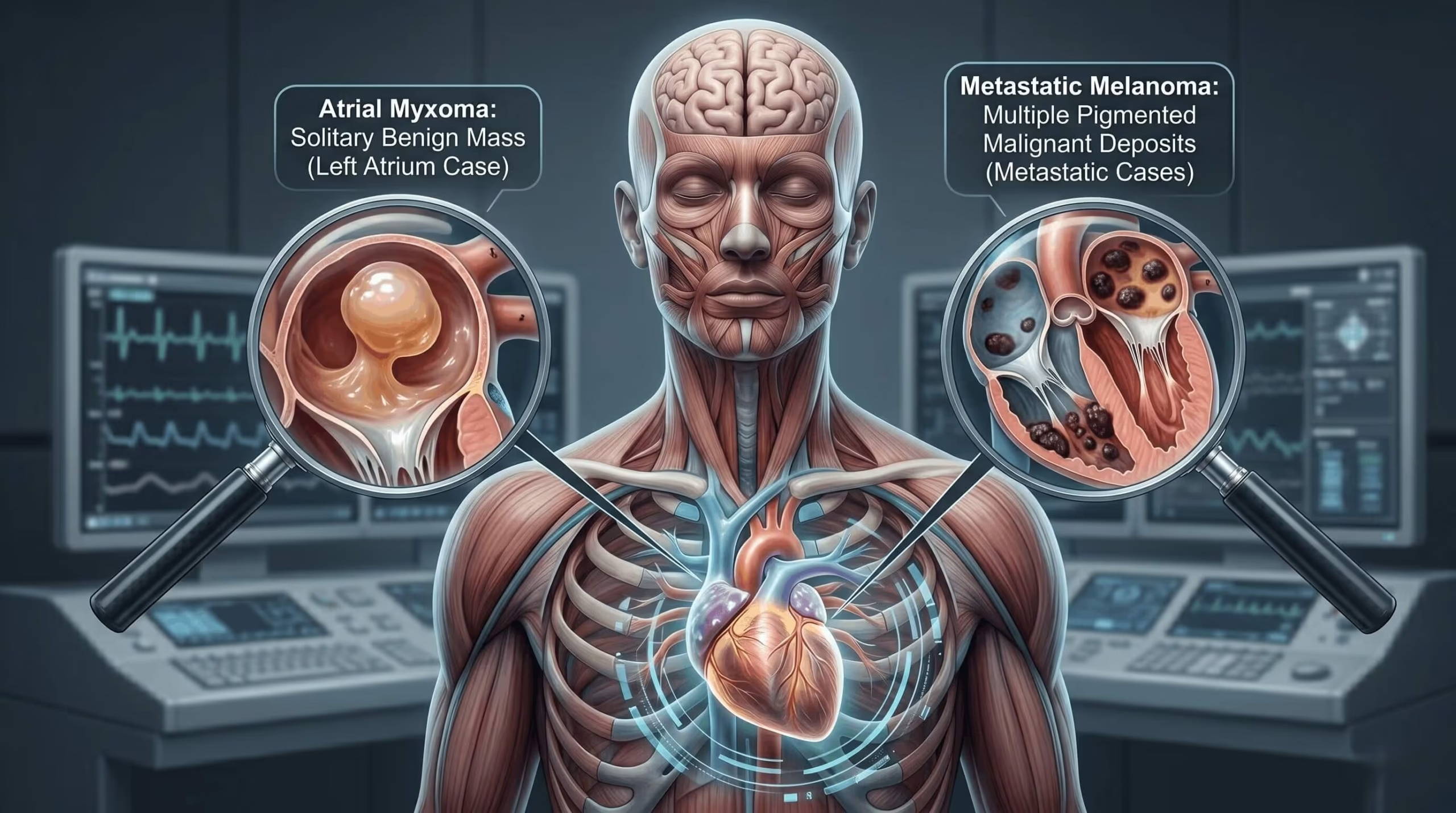
Cardiac masses are uncommon but clinically important — they can embolise to the brain and cause stroke, often in patients with no other conventional cardiovascular risk. Echocardiography is the first-line imaging test for detecting, characterising, and guiding management of cardiac masses. The two cases below illustrate opposite ends of the spectrum: a benign primary cardiac tumour in a young man presenting with palpitations, and a metastatic malignancy in an older patient presenting with stroke.
What These Cases Illustrate
- Cardiac masses can be primary (benign or malignant) or metastatic
- Not every intracardiac mass is a tumour — thrombus and vegetation are important differentials
- Presentation is often non-specific: palpitations, embolic stroke, or incidental finding
- Echocardiography detects and characterises most cardiac masses
- Surgical resection is curative in benign primary tumours such as myxoma
- Metastatic cardiac involvement almost always signals advanced systemic disease
Background on Cardiac Masses
Primary cardiac tumours are rare, with an autopsy prevalence of less than 0.1%. Around 75% of primary tumours are benign — most commonly myxoma. Metastatic involvement of the heart is 20–40 times more common than primary malignancy; lung, breast, melanoma, and lymphoma account for most cardiac metastases.
Cardiac masses broadly fall into four groups: benign primary tumours (myxoma, papillary fibroelastoma, rhabdomyoma, fibroma); malignant primary tumours (angiosarcoma, rhabdomyosarcoma, primary cardiac lymphoma — all rare); metastatic lesions from extracardiac malignancy; and non-neoplastic mimics such as intracardiac thrombus and infective vegetation. Thrombus and vegetation deserve particular emphasis — in everyday practice, they are among the most common causes of an apparent "cardiac mass" on echocardiography, and distinguishing them from true neoplasm is often the clinical task at hand.
- Cryptogenic stroke, particularly in a patient with no atrial fibrillation and no significant carotid disease
- Constitutional symptoms — fever, weight loss, fatigue — classically described with myxoma
- Position-dependent symptoms — dyspnoea or syncope worsening with posture (pedunculated mobile masses)
- Known extracardiac malignancy in a patient with new cardiac symptoms
- Non-specific palpitations or a new murmur in an otherwise healthy young patient
Transthoracic echocardiography is the initial modality in almost all cases. Transoesophageal echocardiography adds detail where TTE is inconclusive, particularly for small masses, attachment points, and prosthetic valves. CT and cardiac MRI provide complementary tissue characterisation when differential diagnosis remains open. For a broader view of echo in stroke workup, see our article on echocardiography in stroke evaluation.
Case 1 — Left Atrial Myxoma in a 38-Year-Old Man
Presentation
A 38-year-old man with no significant medical history presented with a several-week history of palpitations. There was no history of syncope, embolic events, or constitutional symptoms. Cardiovascular examination was unremarkable. Resting ECG showed sinus rhythm, and routine bloods were normal.
Echocardiographic Findings
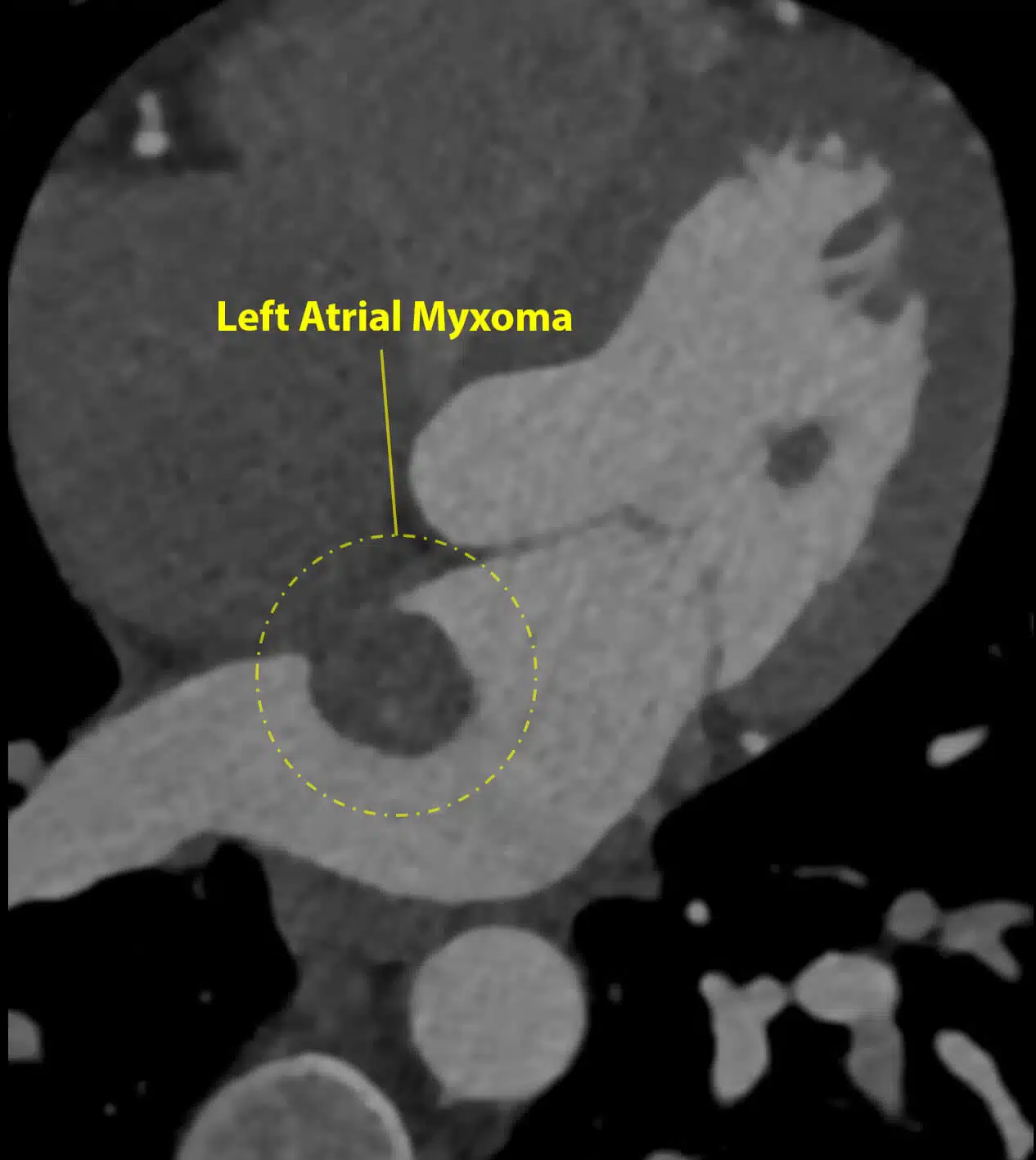
Transthoracic echocardiography revealed a large, mobile mass in the left atrium, attached to the atrial wall by a discrete stalk. Several loosely attached fragments were visible at the surface of the mass, raising immediate concern for embolic risk. Left ventricular size and function were normal; there was no significant valvular disease.
Further Imaging
A CT coronary angiogram was performed to exclude concomitant coronary disease prior to surgery and to better delineate the mass attachment.
Surgical Management
Given the high embolic risk from the mobile fragments, the patient was referred for urgent surgical resection. The mass was removed en bloc along with its attachment site on the atrial wall. The specimen was fragile and required careful handling to avoid fragmentation during excision.
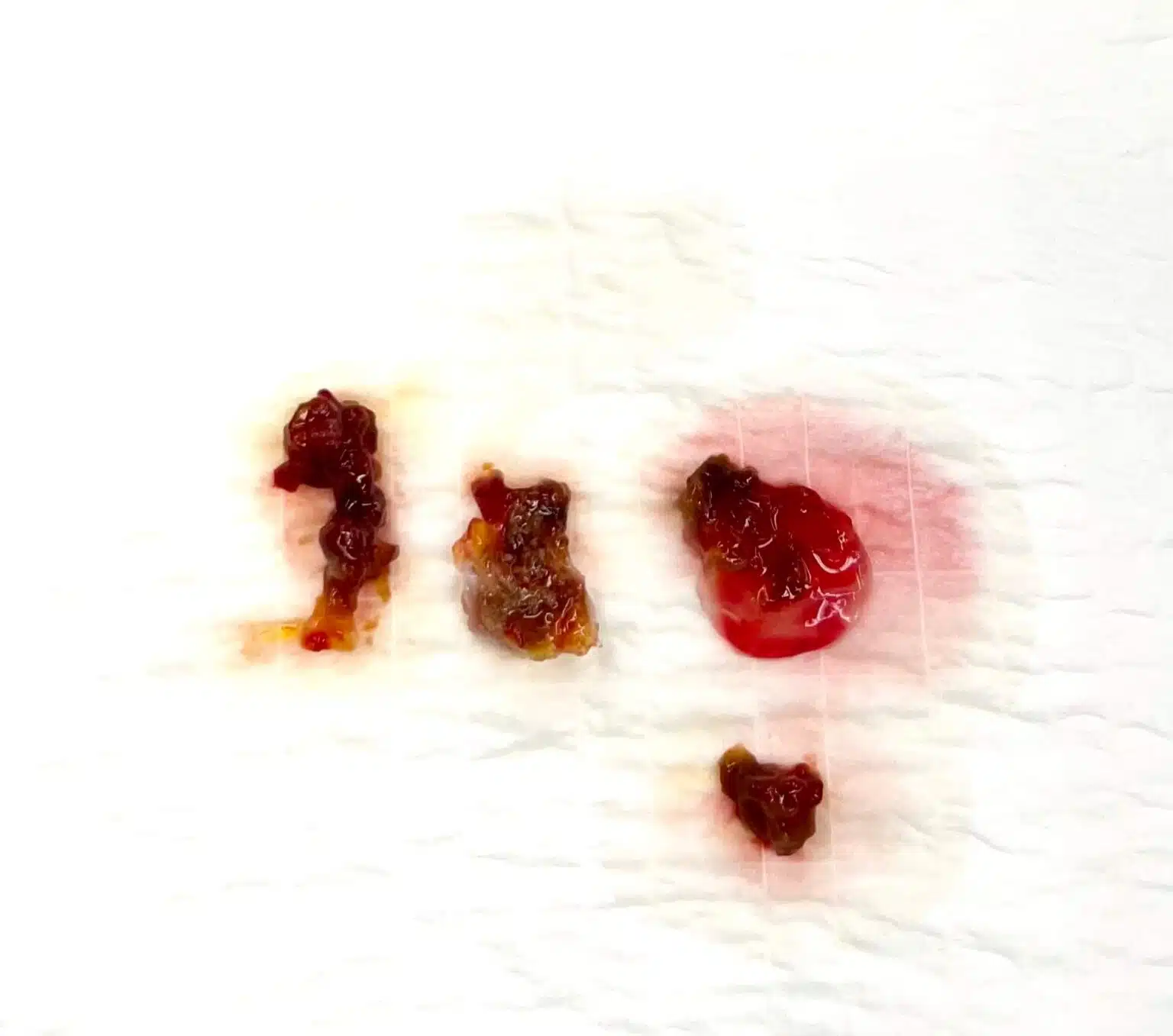
Pathology and Outcome
Histopathology confirmed a benign atrial myxoma. Post-operative recovery was seamless and without complications. Surveillance echocardiography at 6 and 12 months showed no evidence of recurrence.
- Myxoma is the most common primary cardiac tumour in adults, typically arising in the left atrium from the interatrial septum near the fossa ovalis
- Presentation is variable — embolic events, obstructive symptoms (dyspnoea, syncope), or constitutional symptoms (the classical "myxoma triad")
- Palpitations alone, as in this case, are an atypical but recognised presentation
- Surgical resection is curative in the overwhelming majority; recurrence rate is under 5%
- Surveillance echo is recommended post-operatively, particularly in familial (Carney complex) cases
Case 2 — Metastatic Melanoma to the Left Ventricle in a 65-Year-Old Man
Presentation
A 65-year-old man presented with acute ischaemic stroke. He had a known history of cutaneous melanoma of the back. On admission, cerebral imaging confirmed an embolic pattern of infarction. Carotid imaging and rhythm monitoring did not identify a source. Transthoracic echocardiography was performed as part of the cardioembolic source workup.
Echocardiographic Findings
TTE demonstrated a mobile mass within the left ventricular cavity, distinct in echogenicity from the surrounding myocardium. The mass appearance, together with the patient's known melanoma, raised immediate suspicion of cardiac metastatic disease.
Why Melanoma and the Heart?
Of all solid malignancies, melanoma has the most pronounced cardiac tropism. Autopsy series consistently report cardiac involvement in up to half of patients dying with disseminated melanoma — far higher than lung, breast, or gastrointestinal malignancy. The mechanism is haematogenous spread, and any cardiac chamber can be involved, though myocardial and endocardial deposits in the ventricles are most frequently described. In this case, the echocardiographic appearance was suspicious for tumour rather than thrombus on tumour surface, although either can contribute to embolic risk; regardless of which component fragmented, the stroke mechanism was presumed direct embolisation from the cardiac mass.
Diagnosis and Outcome
The combination of known cutaneous melanoma and a new intracardiac mass in the setting of embolic stroke was considered diagnostic of metastatic melanoma with cardiac involvement. Further imaging confirmed metastatic disease beyond the heart. The patient was transitioned to oncology care for immunotherapy; longer-term clinical outcome is not known to the author.
- Metastatic involvement of the heart is more common than primary cardiac malignancy
- Melanoma has a particular tropism for the heart — cardiac metastases are found at autopsy in up to half of patients with disseminated melanoma
- Cardiac metastatic disease almost always reflects advanced systemic disease and is rarely resectable
- Embolic stroke can be the presenting feature, even before other systemic symptoms
- Echocardiography plays a key role in confirming clinical suspicion when a known extracardiac malignancy meets a new embolic event
Comparing the Two Cases
These two cases sit at opposite ends of the cardiac mass spectrum: one benign and curable, the other metastatic and systemic. Together they illustrate why echo findings must always be interpreted in clinical context — the imaging features, the patient's age, and the background history shape the differential as much as the mass itself.
| Feature | Case 1 — Myxoma | Case 2 — Metastatic melanoma |
|---|---|---|
| Age | 38 | 65 |
| Presenting symptom | Palpitations | Embolic stroke |
| Mass location | Left atrium | Left ventricle |
| Attachment | Pedunculated, atrial wall | Infiltrative / mural |
| Echo appearance | Mobile, fragmented surface | Mobile, distinct echogenicity from myocardium |
| Nature | Benign primary | Metastatic malignant |
| Management | Surgical resection | Systemic oncology care |
| Prognosis | Excellent; curative | Reflects advanced systemic disease |
How Echo Helps Distinguish Benign, Malignant, and Metastatic Masses
No single echocardiographic feature is pathognomonic, but the combination of location, attachment, mobility, and tissue behaviour narrows the differential substantially.
| Feature | Benign primary (e.g. myxoma) | Malignant primary | Metastatic |
|---|---|---|---|
| Typical chamber | Left atrium (>75% of myxomas) | Right-sided cavities often; any chamber | Any chamber; pericardium commonly involved |
| Attachment | Discrete stalk — usually interatrial septum near fossa ovalis | Broad-based, infiltrative | Mural, infiltrative, or pericardial |
| Mobility | Often highly mobile | Mass may be fixed or partially mobile | Variable; mural lesions often fixed |
| Surface | Can be friable; fragments visible | Irregular, often with necrosis | Irregular; surface thrombus possible |
| Myocardial infiltration | Absent | Present | Present — often from pericardium inward |
| Pericardial effusion | Uncommon | Common — often haemorrhagic | Very common |
| Number of lesions | Usually single | Usually single | Often multiple |
| Clinical context | Young patient, isolated finding | Constitutional symptoms; aggressive course | Known extracardiac malignancy |
Where echocardiography cannot confidently characterise a mass — particularly when tissue characterisation or infiltration pattern matters — cardiac MRI is the investigation of choice. CT complements when coronary anatomy or extracardiac staging is relevant.
Clinical Pearls
- Every cryptogenic stroke workup should include echocardiography; any intracardiac mass identified warrants further characterisation with TOE and usually cross-sectional imaging
- Context matters as much as imaging — a new cardiac mass in a patient with known extracardiac malignancy is metastatic until proven otherwise
- Urgency of surgical referral in myxoma depends on embolic risk: large size, mobility, and surface fragmentation all raise urgency
- Timing of echo after stroke is ideally early, as some masses (particularly fragile ones) can embolise further within days
- In endocarditis workup, the differential between vegetation and tumour often requires TOE and should be discussed with the treating team before committing to a diagnostic label
- Cardiac masses are uncommon but an important and often treatable cause of embolic stroke.
- Myxoma is the most common primary cardiac tumour in adults; surgical resection is curative.
- Metastatic cardiac involvement is far more common than primary cardiac malignancy and usually signals advanced systemic disease.
- Thrombus and vegetation are important non-neoplastic differentials for any apparent cardiac mass.
- Echocardiography is the first-line investigation; TOE and cardiac MRI provide complementary detail.
- Clinical context — a known malignancy, or a cryptogenic embolic event — often shapes interpretation as much as the imaging appearance.
Frequently Asked Questions
What is a cardiac myxoma?
A myxoma is a benign primary tumour of the heart, most commonly arising in the left atrium. It can cause stroke through embolisation, or obstructive symptoms through interference with blood flow, and is usually curable with surgical resection.
How are cardiac masses detected?
Transthoracic echocardiography is the first-line test. Transoesophageal echocardiography, cardiac CT, and cardiac MRI provide complementary detail when characterisation is uncertain.
Can cancer spread to the heart?
Yes. Metastatic cardiac involvement is far more common than primary cardiac tumours. Melanoma, lung, breast, and lymphoma are the main culprits, with melanoma showing a particularly strong tendency to involve the heart.
Why does a cardiac mass cause stroke?
Fragments of the mass, or blood clots that form on the surface of the mass, can break off and travel through the arterial circulation to the brain, causing embolic stroke. In some cases the stroke is the first clinical manifestation of the cardiac mass.
Is every intracardiac mass a tumour?
No. Thrombus (blood clot) and infective vegetation are common non-neoplastic differentials, and in everyday practice they are more frequent than true tumours. Distinguishing them relies on imaging appearance combined with clinical context.
Conclusion
These two cases illustrate the diagnostic range of cardiac masses — from a curable benign tumour in a young patient to metastatic malignancy in an older one — and the central role echocardiography plays in identifying both. In any patient with a cryptogenic embolic event, or a known malignancy with new cardiac symptoms, the question of a cardiac mass should be actively asked and answered with imaging.
Cases presented are fully de-identified and shared for educational purposes only. No patient-identifying information is included.